
If you thought fintech was cool, wait until you hear about femtech: cutting-edge, high-tech ob/gyn treatment. Originally devised as a way to keep patients and physicians safe during COVID, femtech will eventually bring first-rate OB/GYN care to women in developing countries.
In just under a year since its opening, the ARC Innovation Center at Sheba Medical Center has been spearheading pioneering innovation in digital health — locally and in collaboration with other top medical centers globally. Last month, ARC@Sheba launched the world’s very first Women’s Health Innovation Center, directed by Dr. Avi Tsur, an OB/GYN and high-risk pregnancy expert, affiliated with Sheba’s Josef Buchmann Gynecology and Maternity Center, directed by Professor Eyal Sivan. Having recently returned from a 3-year stint at the prestigious Stanford Medical Center where he was a visiting clinical fellow and research fellow, Dr. Tsur says that the brand-new Women’s Health Innovation Center will provide women from across the country with quality OB/GYN medical treatment via the latest high-tech solutions employing artificial intelligence, telemedicine, precision medicine and more.
“Providing remote health care with the use of telemedicine will enable us to ensure the safety of our patients in the era of COVID-19 – but regardless, it’s certainly better for a woman to monitor herself at home for 10 minutes than to have to wait for 4 hours in the clinic,” said Dr. Tsur. “In terms of our long-term goals, it will enable also women who live at a distance to be able to benefit from our treatment.”
With the help of the very latest, cutting-edge technologies for remote health care, the center will deal with various categories of women’s health, including high-risk pregnancies, postpartum follow-up, contraception, IVF, gynecological oncology and more.
At the event launching the center, Dr. Tsur presented many of the new technologies, explaining how his team integrates solutions developed by different startups. “For each specific field, we first perform a pilot study to see how the technology plays out in the clinical setting. Depending on the circumstances, patients can now have part of all of their ‘visits’ performed from home.”
Many doctors have mixed feelings about treating patients remotely, and Dr. Tsur is no exception. “Telemedicine creates new challenges because part of our clinical skill depends on being in the same room with the patient. I think that we need to leverage the new technology so as to overcome the associated disadvantages,” he said, clarifying that at the end of the day, it’s about providing patients with the best treatment. “Clearly, we will never compromise; telemedicine is meant to enhance treatment; when the need arises, we will convert a telemedicine visit to a real visit.”
Dr. Tsur conveys his excitement with the center’s many new projects, devising solutions to new and old problems. One example: an AI model that Dr. Tsur developed together with Dvir Aran, a data scientist (PhD) from the University of California, San Francisco, to predict shoulder dystopia in labor. “Until now, this potentially life-threatening complication was considered unpredictable, but we developed a technological model to predict it. We were then able to validate that model with our ongoing collaboration with Stanford, the University of Texas, and UCSF.”
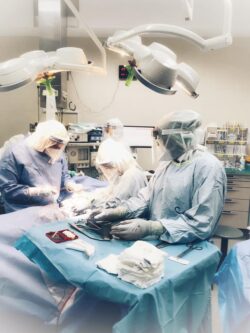
Dr. Tsur during COVID-19 C-section. “Even in the era of maternal-fetal telemedicine, some things will still need to be done in person.”
According to Dr. Tsur, that collaboration doesn’t end there. “We can also develop various high-tech solutions one step further using AI, extended reality and other tools. That’s the most exciting aspect of collaboration.”
At the launching event of the Women’s Health Innovation Center, Dr. Tsur described the various high-tech gadgets that enable women with high-risk pregnancies the luxury of staying at home to self-monitor. “Remote monitoring of vital signs, blood count- and glucose monitoring, fetal monitoring and sonographic evaluation all reduce the need for high-risk and post-date pregnant women to attend the clinic in person, while the situation is constantly assessed either by AI methods or by an obstetrician who is online,” he said.
One of the inherent challenges is responding to a deceleration in fetal heartbeat when the woman is not in a hospital setting. “But that is no different from a situation where a woman would be monitored at an outpatient clinic,” Dr. Tsur pointed out. In both instances, she would be rushed to the hospital if the need arose.
Another pilot study involves discharging women about eight hours after delivery, instead of the usual 36 to 48 hours. The pilot is investigating a comprehensive telemedicine solution aimed at replacing hospitalization with at-home follow up and early detection of the most common postpartum complications— surgical wound infection, thromboembolic complications, breastfeeding difficulties and postpartum depression.
The concept of telemedicine is generally thought of as a diagnostic tool between the physician and the patient. But one of Dr. Tsur’s pilots involves a system that enables image-sharing between physicians. Thus, an obstetrician performing an ultrasound in one venue can share the imaging online, in real-time, with top experts anywhere in the world, who can then offer guidance, such as for better positioning and the like.
Plans are in the pipeline for various other projects, including gynecological oncology remote evaluation, a pilot to be led by Dr. Jacob Korach employing an AI-enabled device for self-examination. The success of these pilots will determine the use of these technologies also in developing countries where women lack access to first-rate medical care.






